The Polarity Perspective
Beyond Split vs. Full-Thickness Graft: Why Traditional Skin Grafts Fall Short in Chronic Wounds
Why Graft Type Matters in the Race
Once a skin graft is placed, it enters a race:
Ischemic injury pushes the graft toward failure
Revascularization pushes it toward survival
But the odds of winning that race are set before the graft ever touches the wound—by graft thickness, donor-site biology, procedural requirements, and patient factors.
Nowhere is this more apparent than in patients with chronic wounds and diabetic foot ulcers (DFUs).
Skin Graft Healing: A Race Against Time
How grafts survive, why they fail, and why chronic diabetic foot ulcers (DFUs) make the race harder
What Is a Skin Graft?
A skin graft is a segment of skin that is completely detached from its original blood supply and transplanted onto a wound bed. Unlike a flap, a graft arrives ischemic—with no active circulation—and must rapidly establish a new blood supply to survive.
This single fact defines everything about skin graft success.
From the moment a graft is harvested, a race begins.
The Central Concept: A Race Between Survival and Death
Skin graft healing can be thought of as a race between two competing forces:
Graft ischemic injury and cell death
Re-establishment of adequate blood supply
Wound Healing Is Not a Moment — It’s a Dynamic Biological Orchestra
A practical refresher on the biology of wound healing and why it breaks down.
Wounds don’t heal by accident. They heal through a tightly regulated, biologically programmed sequence of events. When that sequence runs smoothly, tissue restores structure and function. When it breaks down, wounds stall … and become chronic.
A few facts worth pausing on
Acute wounds are biologically “time-limited” and they are meant to heal. Chronic wounds are not simply slow wounds; they are biologically different. Most chronic wounds are
Skin Is Not a Covering — It’s a Regenerative Organ
The skin is often treated like a passive wrapper - something that tears, breaks down, or “fails to heal.” In reality, it’s one of the most dynamic, biologically active organs in the human body.
A few facts to reset the frame:
Skin is the largest organ in the human body, making up ~15–20% of body weight
The epidermis fully renews every ~28–40 days in healthy adults
Tens of thousands of skin cells are shed every minute
Up to one-third of cardiac output can be directed to the skin at rest
Skin is the first immune organ to encounter trauma, pathogens, and environmental stress
What Does “Regenerative” Actually Mean in Wound Care?
The word regenerative has become ordinary in wound care. It appears in scientific literature, conference presentations, marketing materials, and everyday clinical conversations. Despite its everyday use, the term isn’t widely understood.
As someone who has spent many years working at the intersection of medicine, science, and commercialization, I believe clarity around this term is important. When we use the word regenerative, we should be explicit about what we mean, and equally clear about what we do not.
Article Review: What Autologous Wound Care Solutions Exist for Full-Thickness Skin Defects?
By Nikolai Sopko, MD, PhD, Chief Scientific Officer & Chief Operating Officer, PolarityBio
In recent posts, we’ve examined two questions that continue to shape modern wound care: whether living cells matter in advanced wound care, and whether the source of those cells—autologous or allogeneic— meaningfully changes the biology of healing.
If you accept that cells matter, and that autologous biology offers unique advantages, the next logical question is a practical one: what autologous wound care solutions are actually available today?
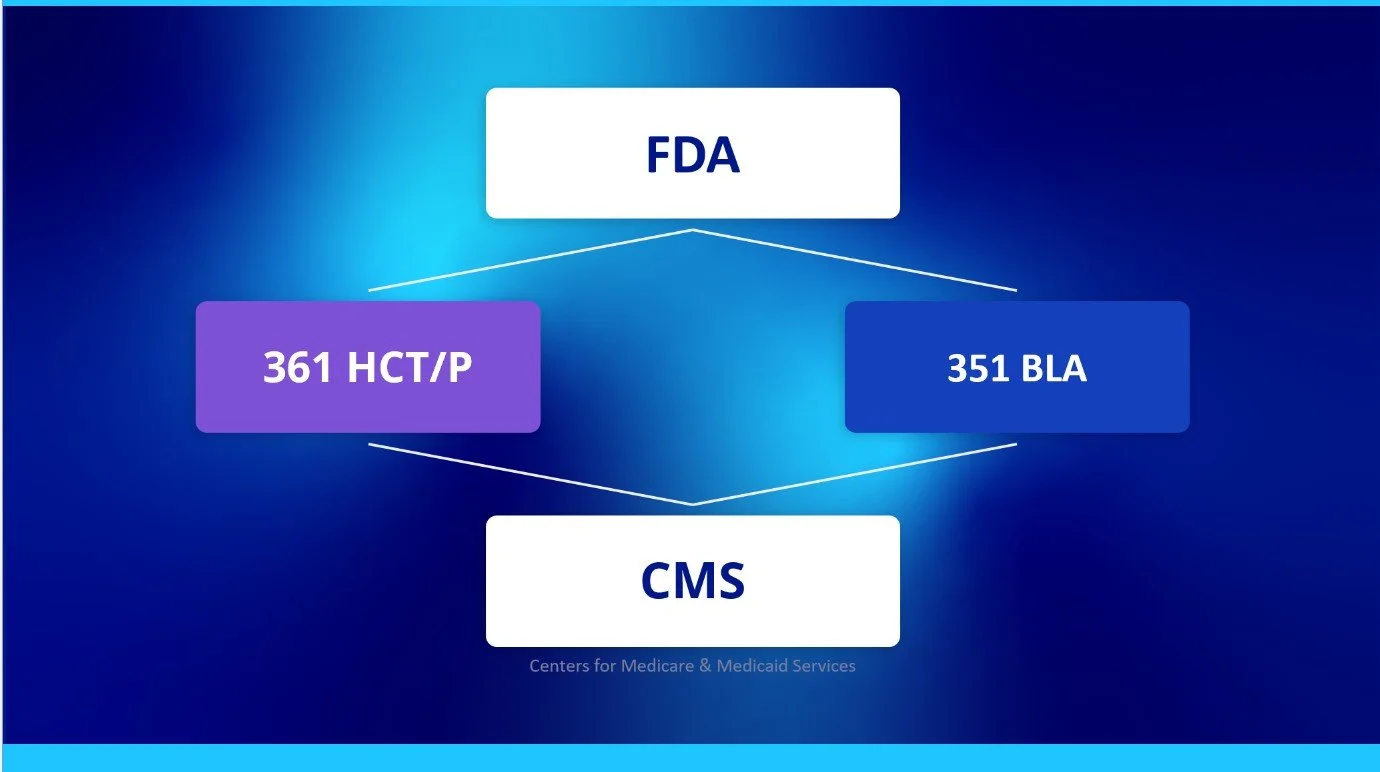
Understanding FDA Pathways for Human Cell and Tissue Products: 361 HCT/P vs. 351 Biologic License Application
By Nikolai Sopko, MD, PhD Chief Scientific Officer & Chief Operating Officer, PolarityBio
In regenerative medicine, products derived from human cells and tissues are regulated under different FDA regulatory pathways depending on their characteristics, intended use, and method of manufacture. Two labels frequently used to describe these pathways are “361” and “351.” These pathways represent distinct regulatory approaches with meaningful implications for product oversight and, now, Medicare payment policy.
Why “Whose Cells” Matters in Regenerative Medicine
By Ned Swanson, MD, President & Chief Medical Officer, PolarityBio.
As regenerative therapies advance in wound care, most conversations center on what a therapy contains - cells, matrix, or signaling components. But there’s another important component - where those elements come from.
The source of tissue matters because it influences how a therapy interacts with the body, how well it’s tolerated, and how closely it mimics natural healing processes. In regenerative medicine, the distinction between autologous and allogeneic approaches is essential.
Cells or No Cells…Understanding Acellular and Cellular Therapies for Wound Healing
By Ned Swanson, MD, President & Chief Medical Officer, PolarityBio.
As regenerative treatments become more common in wound care, one distinction is critical: cellular versus acellular therapies. These terms often get used interchangeably, but biologically they represent very different approaches. Understanding that difference is key to knowing whether a therapy can truly support tissue regeneration.